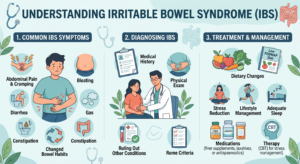
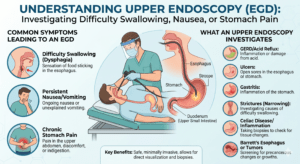
What is Barrett’s Esophagus?
In order to understand Barrett’s esophagus it is useful to understand the normal appearance of the esophagus. In a normal esophagus, the tissue lining appears pale pink and smooth. These flat square cells, called “squamous” cells, make up the normal lining of the esophagus. See illustraion A below.
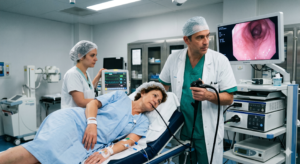
In contrast, Barrett’s esophagus is a salmon-colored lining in the esophagus, made up of cells that are similar to cells found in the small intestine and are called “specialized intestinal metaplasia”. Illustration B shows what Barrett’s esophagus looks like at endoscopy (a small flexible scope with a camera in its tip).
he reason Barrett’s esophagus is important is because people who have it have a small increased risk of developing esophageal cancer. Barrett’s esophagus and heartburn symptoms are associated with a specific type of esophageal cancer called “esophageal adenocarcinoma.”
How Common is Barrett’s Esophagus?
Barrett’s esophagus is more commonly seen in people who have frequent, persistent heartburn or gastroesophageal reflux disease (GERD). GERD symptoms include heartburn (burning under your breast bone) that may wake you up at night, occur after meals or in between, and may temporarily improve with antacids. Acid regurgitation, or the experience of sour or bitter tasting fluid coming back up into your mouth, is also a GERD symptom. Some people do not have any of these symptoms and are still at risk of developing Barrett’s esophagus.
What are the Risk Factors for Barrett’s Esophagus?
Age, male sex, Caucasian ethnicity and GERD symptoms of longer than 10 years duration are risk factors for Barrett’s esophagus. GERD, tobacco smoking, and obesity are risk factors for developing esophageal carcinoma. Tobacco use (especially chewing tobacco) and drinking alcohol are much stronger risk factors for a different type of cancer, squamous cell cancer of the esophagus. Tobacco slightly increases a person’s chance of developing esophageal adenocarcinoma, but this risk is increased when the person already has Barrett’s esophagus.
Most people with Barrett’s esophagus are in their 60’s at the time of diagnosis. It is thought that most people who are diagnosed with Barrett’s have had it for 10 to 20 years before diagnosis.
Males are 3 to 4 times more likely to have Barrett’s esophagus compared to females. Caucasians are about 10 times more likely to have Barrett’s esophagus than persons of African American ethnic background.
Although people who experience weekly heartburn or acid regurgitation are 64 times more likely to get esophageal adenocarcinoma than people who have never experienced these symptoms, 40% of people with esophageal adenocarcinoma deny ever experiencing GERD symptoms. Why these people developed esophageal adenocarcinoma remains a mystery.
What are the Treatment Options for Barrett’s Esophagus?
Generally, doctors treat the symptoms of GERD, not Barrett’s esophagus, specifically. Barrett’s is an acquired disorder, meaning it develops over time and is not present at birth. It is usually diagnosed around age 60, although we estimate that half of people with Barrett’s esophagus have it by age 40.
Treatment for GERD symptoms are listed in the GERD section of this web page and elsewhere on the ACG Web Book for patients. Generally this will include antacids, histamine receptor antagonists and proton pump inhibitors. Surgery is also an option. The large majority of patients with Barrett’s esophagus will be treated with a proton pump inhibitor.
The proton pump inhibitors (PPIs) include: esomeprazole (Nexium), lansoprazole (Prevacid), omeprazole (Prilosec), pantoprazole (Protonix), rabeprazole (Aciphex) and omeprazole powder (Zegerid). With regard to the optimal way to take a proton pump inhibitor, you should take your medication half an hour before a meal. Most other pills can be taken along with PPI’s, except for antacids, carafate, and questran. Antacids, Carafate® and Questran® bind almost everything they come in contact with, so, if you are on these medicines, you should not be taking them at the same time as other medicines in the first place!
PPIs work by turning off the cellular pumps in your stomach that make acid. Eating food 20 to 60 minutes after taking your pill on an empty stomach activates millions of these acid pumps which are then turned off by the medication. This is the key for optimal dosing of a PPI.
When Should You See a Doctor about Barrett’s Esophagus?
You should see a doctor if you have the risk factors listed earlier (male sex, age 50 or over, Caucasian ethnic group, GERD symptoms of longer than 10 years duration). If you have alarm symptoms such as trouble swallowing, losing weight without trying, blood in your stool, persistent symptoms despite medical therapy, or new chest pain, you should discuss your symptoms with our doctor and have an endoscopic examination.
What Type of Tests are Needed to Evaluate Barrett’s Esophagus?
Endoscopy is the test of choice for Barrett’s esophagus. At endoscopy, biopsies can be taken; meaning small pieces of tissue can be collected to look at under the microscope. In Barrett’s, tissue is the issue. Tissue, showing intestinal metaplasia with goblet cells, is necessary to make the diagnosis of Barrett’s esophagus, and is one of the keys to management of Barrett’s.
An upper GI barium study is helpful in finding strictures (areas of narrowing), usually causing trouble swallowing. Barium studies are not useful for diagnosing Barrett’s esophagus, because it is a microscopic diagnosis.
Management of Barrett’s esophagus?
At endoscopy, our doctor will get multiple biopsies every 1 to 2-cm (one half to one inch) along the length of your Barrett’s esophagus segment. How the biopsies look on a microscope slide influences your management.
The key to the management of Barrett’s esophagus is the level of dysplasia that the biopsies show. “Dysplasia” is the Greek word for “change”; a reflection of how disordered and disorganized the cells are.
All of our cells are programmed to die. We are constantly making new cells while old cells slough off. For example, dandruff is old dead scalp cells that have dried up and flaked off. Just like your skin on the outside of your body, the lining of the esophagus is skin on the inside of your body. Cells keep their DNA in their nucleus. Cancer is DNA that has lost control causing cells to forget how to die. In cancer, cells grow and grow without dying.
When cells are changing from normal to cancer, they go through steps called dysplasia.If a diagnosis of Barrett’s esophagus is made, ideally there should be NO dysplasia.
In biopsies with no dysplasia, the nuclei are small, organized and located at the base (bottom) of the Barrett’s cell. Most people with Barrett’s esophagus will need to undergo future endoscopies to assure there is no progression of the condition. Follow up endoscopy for Barrett’s without dysplasia is usually recommended at 3 years, but our doctor will help decide what is most appropriate for you.
If biopsies are found to have low-grade dysplasia, where the nuclei are still small but somewhat disorganized, our doctor will recommend you undergo a repeat endoscopy in about 6 months.
High-grade dysplasia is thought to be the stage that occurs before esophageal cancer. However high-grade dysplasia can regress to low-grade dysplasia. If diagnosed with high-grade dysplasia the biopsies whould be examined again by a pathologist who specializes in diseases of the esophagus. Pathologists are physicians that are experts at examining tissue on microscope slides.
If a diagnosis of high-grade dysplasia is confirmed, there are 4 management options:
- Esophagectomy. This is a major surgery where a surgeon removes the esophagus and hooks up the stomach to the very top of the remaining swallowing tube. It has been shown that experienced esophagus surgeons that do the most esophageal surgery have the best outcomes and lowest death rates. Surgery is the standard-of-care.
- Increase your acid suppression medications, and have another endoscopic examination in 3 months. This time, our doctor will get more biopsies, 4 every single centimeter (half inch) along the length of the Barrett’s segment. If you have a nodule or bump inside the Barrett’s segment, our doctor may recommend having an “Endoscopic Mucosal Resection” to shave off that bump and make sure it is not cancer. You may also undergo an endoscopy with ultrasound to look for deeper extension of the bump or lymph nodes.
- Photodynamic Therapy and other ablative techniques. These are currently considered research and experimental but, for very specific patients, may be an excellent option. There are specific doctors that have expertise in these treatments. If you are interested, you should find the expert in your area, and consider being enrolled in a study, to have this done.
- In photodynamic therapy, you get an injection in your vein of a medicine that deposits in the skin (inside – in the esophagus, and outside – on the part that sees the sun). Then, during endoscopy, a laser beam light is shined in your esophagus. The light causes the chemical to kill the cells of your esophagus lining, and you pass them from below in a bowel movement. The complications of this procedure include formation of esophageal strictures, and sun-sensitivity that may limit your ability to spend time in the outdoors for about 6 weeks. The benefit of this type of procedure, if it worked, would be avoidance of surgery.